If you work in healthcare, you’ve probably noticed more conversation around non-pharmaceutical treatment options in recent years. Patients are asking more questions, pushing back on medication-heavy approaches, and actively seeking alternatives for pain management and tissue recovery. Frequency Specific Microcurrent (FSM) therapy — a technique that uses extremely low-level electrical currents to support healing — is one of the tools practitioners are starting to look at more seriously.
The technology isn’t new. Frequency-specific microcurrent devices have been used in clinical settings since the 1980s, and the underlying science goes back even further. What’s changed is a combination of growing research, a rise in patient demand for non-invasive options, and a new generation of devices that are significantly easier to integrate into an existing clinical practice.
The Pain Problem Driving Demand
Chronic pain is one of the most pressing challenges facing modern healthcare. According to a 2024 report from the National Center for Health Statistics, 24.3% of U.S. adults reported chronic pain in 2023 — up 18% from 2019. That represents roughly 60 million people, many of whom are actively seeking options that go beyond standard pharmaceutical approaches and conventional pain management.
How Microcurrent Therapy Works
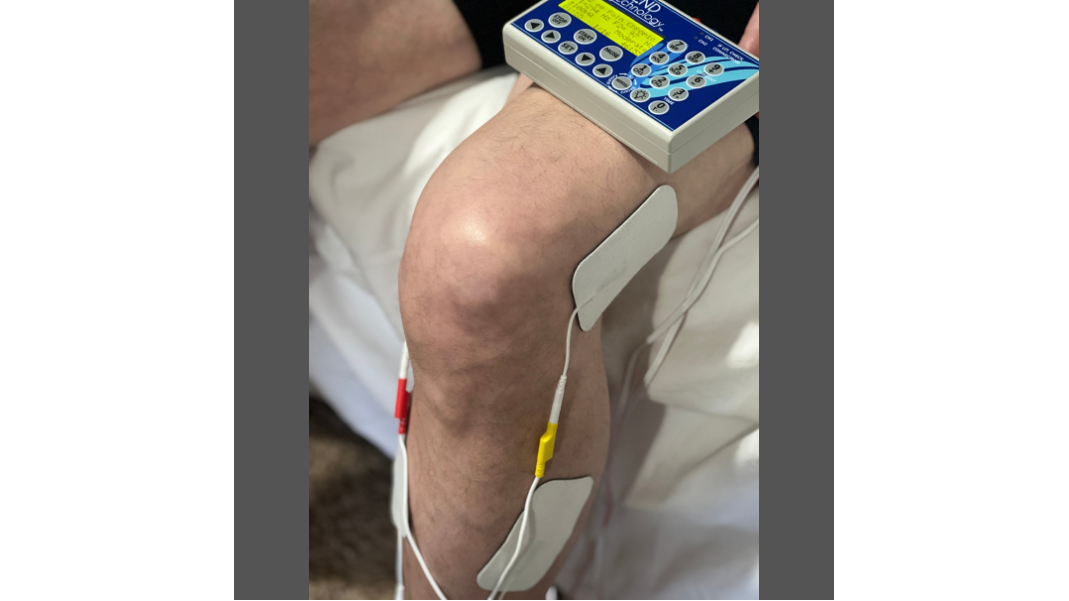
Microcurrent therapy delivers electrical current in the microampere range — roughly one-thousandth the intensity of standard TENS units. Because the current operates close to the body’s own bioelectrical signals, most patients feel nothing during a session. Research suggests it may support cellular ATP production and promote tissue repair. The FDA has cleared microcurrent devices for pain management as a safe adjunct to primary care.
What Practitioners Are Actually Looking For
For clinicians thinking about adding this modality, the practical questions matter just as much as the clinical ones. Can the device run automated protocols without constant manual adjustment? Can it be customized for different patient conditions? Is it portable for the way your practice operates? A device that runs pre-loaded protocols frees the practitioner to focus on the patient, not the equipment.
Getting Started Without Getting Overwhelmed
One barrier to adoption has always been the learning curve. Building effective protocols from scratch takes time and experience, and not every practitioner who is new to the field has that background quite yet. Some manufacturers now offer pre-loaded protocol libraries, which help newer practitioners get started without designing programs from scratch and allow them to test the therapy before committing to custom workflows.
Is It Right For Your Practice?
The decision to add any modality comes down to patient population, workflow fit, and realistic expectations. Microcurrent works best as a complement to established care, not a substitute. Practitioners apply it for musculoskeletal pain, nerve-related discomfort, and post-injury recovery. Practitioners most often look for flexible equipment that can handle both manual and automated treatment in a single unit — a practical consideration worth weighing before committing to any device.
For practices that haven’t yet added it, microcurrent therapy is worth taking seriously as patient demand for non-pharmaceutical care continues to grow. Understanding how the technology works — and knowing what to look for in a device — makes it considerably easier to decide whether it fits your practice and your patient population.
MEND Technology
6715 NE 63rd St
Ste 103 PMB 120
Vancouver
Washington
98661
United States
